
Medicare Enrollment Periods may be complicated. But its important to stay informed and up-to date on enrollment periods to avoid penalties or coverage gaps.
There are 6 different Medicare Enrollment Periods including the following:
- Initial Enrollment Period
- General Enrollment Period
- Annual Enrollment Period
- Open Enrollment Period
- Medigap Open Enrollment Period
- Special Enrollment Period
1. Medicare Initial Enrollment Period
If you’re about to turn 65 and are newly eligible for Medicare, this is your gateway to start receiving your Medicare benefits. If you have a disability, end-stage renal disease (ESRD) or
ALS (also called Lou Gehrig’s disease), you may be eligible for Medicare even before you turn 65.
The Initial Enrollment Period (IEP) is a seven-month window that enables you to enroll in Medicare if you’re about to turn 65, still working, and not yet getting social security or railroad benefits.
If you’re already receiving social security or railroad benefits, you’ll be automatically enrolled in Medicare Parts A and B.
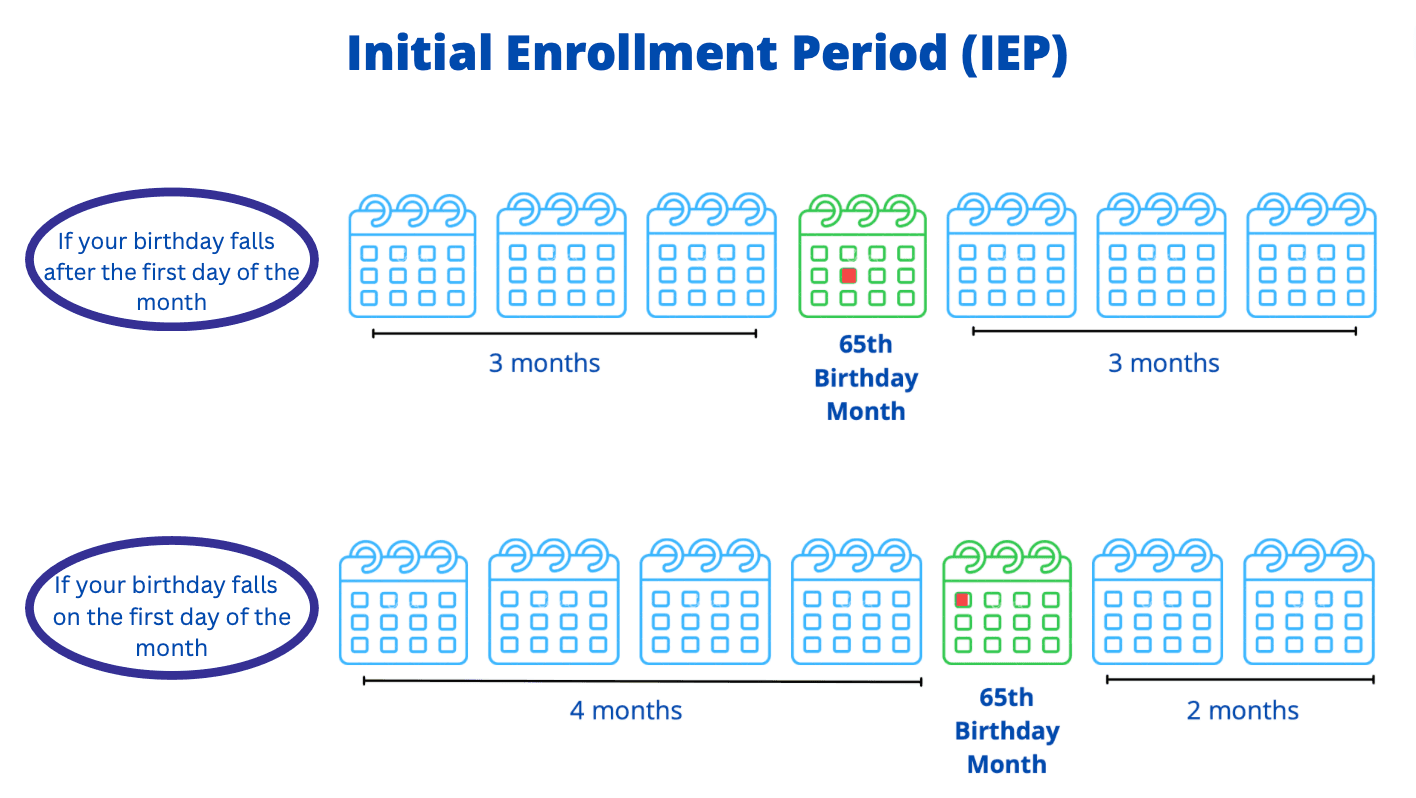
The IEP depends on your date of birth
- If your birthday falls on the first of the month, it begins 4 months before your birth month and extends until 2 months after your birth month; otherwise…
- It begins 3 months before your birth month and extends until 3 months after your birth month
For example, if your birthday falls in February, your IEP starts in November and ends in May. But if your birthday is on the 1st of February, your IEP begins in October and ends in April.
During your IEP, you can:
- Enroll in Original Medicare (Part A and Part B)
- Enroll in Medicare Part D (Medicare prescription drug plan)
- Enroll in Medicare Part C (Medicare Advantage Plan)
Failing to enroll during this 7-month Initial Enrollment Period may result in a monthly late enrollment penalty for as long as you have Part B coverage. In addition, you may incur a Part A penalty if you have to pay a Part A premium.
2. General Enrollment Period
The General Enrollment Period runs from January 1st to March 31st and is the time you can enroll in Medicare Part A and B if:
- You missed enrolling in Medicare during your IEP
- You don’t qualify for a Special Enrollment Period
If you’re enrolling in Medicare during the General Enrollment Period, your coverage will begin the following month after you sign-up.
You may incur late penalties for the duration of your enrollment in Medicare if you don’t enroll in time. So, in addition to paying your regular premiums for Part B (and Part A, if applicable), you’ll also have to pay a late penalty as long as you remain enrolled in Medicare.
3. Medicare Annual Enrollment Period
Once you have enrolled in Medicare, you do have the right to make changes each year. From October 15th to December 7th, the Medicare Annual Enrollment Period allows you to make changes to Part C and Part D.

At this time you can:
4. Medicare Advantage Open Enrollment
From January 1st to March 31, you can change your Medicare Advantage plan for any reason.
During this time, you can:
Yes, you can drop a Medicare Advantage plan and return to Original Medicare, but there are no guarantees on a Medigap plan. Remember that carriers will ask health-related questions and can choose to not enroll you.
5. Medigap Open Enrollment Period
If you plan to supplement your Original Medicare coverage with a Supplemental Plan or a
Medigap plan, the best time to do this is during the Medigap Open Enrollment Period.
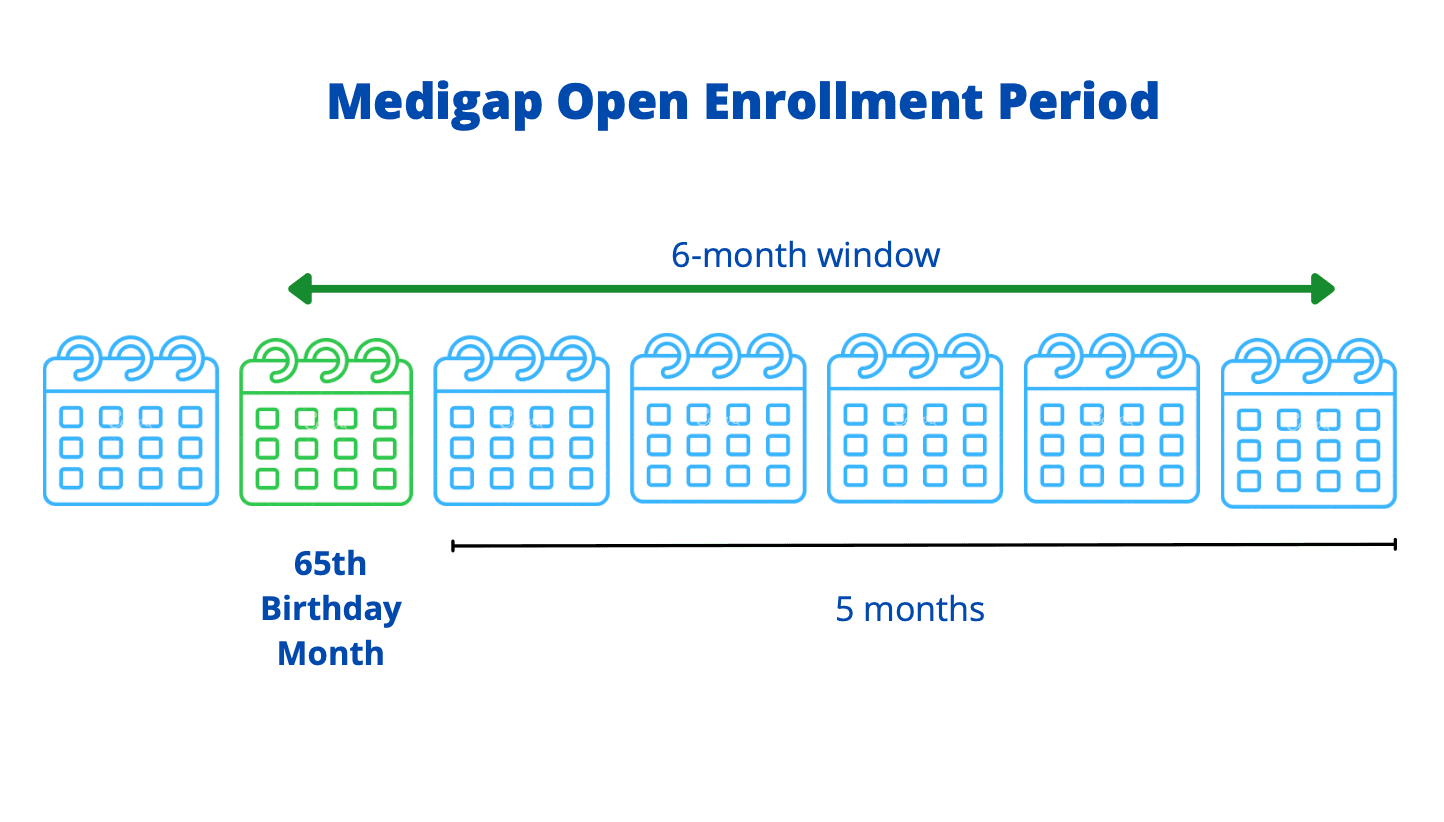
The Medigap Open Enrollment Period is a 6-month window that starts from the month you turn 65 and have Medicare Part B and ends 5 months after your birth month. For example, if your 65th birthday falls in February, your Medigap Open Enrollment Period begins in February and extends until July.
During the Medigap Open Enrollment Period, you’ll typically get better pricing and a wider choice of Medigap plans, regardless of your health status. You can purchase any plan offered in your state without undergoing medical underwriting.
Note: if you choose to enroll in a Medigap plan outside your Medigap Open enrollment period, insurance companies may use medical underwriting to decide whether to accept your application (and how much to charge you for the plan) unless you have Guaranteed Issue Rights.
6. Special Enrollment Period
Medicare beneficiaries may be able to make changes to their existing Medicare health and drug coverage outside the regular enrollment periods if they qualify for the Special Enrollment Period.
You’re eligible for the Special Enrollment Period if:
- You move to a different location
- You lose your current coverage
- You have a chance to get other coverage
- Your plan changes its contract with Medicare
- The state you live in grants SEPs
During the Special Enrollment Period, you can join, switch or drop a Medicare Advantage Plan or a Prescription Drug Plan.
You can go to the Official Website for Medicare at www.medicare.gov for more information about joining a plan and when to join.
